The latest news from Europe
Provided by AGPHow strokes that trigger psychiatric symptoms are guiding new approaches to brain stimulation therapy
Focal brain injuries that produce psychiatric syndromes overnight are revealing the distributed networks whose disruption causes suffering.
The important questions demand patience, nuance, and a willingness to revise assumptions. The field should stay accountable for whether our research helps explain suffering and improve people's lives.”
NEW YORK, NY, UNITED STATES, May 5, 2026 /EINPresswire.com/ -- Consider, for a moment, the man who went to bed himself and woke up someone else. He had a small stroke in the night. Nothing dramatic. A pinprick of damage in a quiet corner of the brain, the kind of injury that on a scan looks almost apologetic. By morning, however, he was a stranger to his wife. Talking too fast. Spending money he did not have. Convinced of his own brilliance in a way that would have been charming if it were not so frightening. He had no history of mental illness. He had a stroke, and the stroke gave him mania.— Gonçalo Cotovio, MD, PhD, Champalimaud Foundation
Or consider the woman who, after a similar accident in a different region of the brain, began washing her hands until they bled. She had never had a compulsion in her life. The lesion handed her one, fully formed, like an unwanted inheritance.
These cases are rare, but they are not curiosities. They are, in the view of one young Portuguese psychiatrist, the closest thing psychiatry has to a smoking gun. And in two papers published this week by Genomic Press, Gonçalo Cotovio of the Champalimaud Foundation in Lisbon argues that the field has been staring at this evidence for decades without quite knowing what to do with it.
Now he thinks he knows.
The argument, set out at length in a Brain Health Viewpoint co-authored with his mentor Albino J. Oliveira-Maia and freely available at https://doi.org/10.61373/bh026v.0012, is at once simple and seismic. Psychiatry, Cotovio and Oliveira-Maia contend, has spent more than a century searching for the brain region responsible for depression, or schizophrenia, or addiction, and finding instead a frustrating tangle of correlations. Brain area X lights up in this disorder. Connectivity pattern Y looks different in that one. The arrows of causation, however, have stayed stubbornly two-headed. Did the brain change cause the illness, or did the illness change the brain? Nobody quite knew.
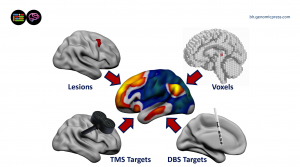
Lesions break the symmetry. When a focal injury arrives on a Tuesday and the obsessions arrive on a Wednesday, the temporal order is no longer a matter of inference. It is on the chart. And when researchers gather enough such cases and ask what the lesions have in common, they discover something that quietly upends the textbooks: the lesions almost never share a location. What they share, instead, is a network. Different injuries, different coordinates, different patients, all of them wired into the same distributed circuit. Damage that circuit anywhere along its length and the same syndrome appears.
Cotovio calls this causal network mapping, and the technique is doing something psychiatry has wanted to do for a hundred years and could not. It is identifying brain circuits that do not merely correlate with suffering but produce it.
"If a focal brain lesion can precipitate a syndrome such as mania or obsessive-compulsive symptoms, the connected network may reveal something fundamental about disease mechanisms," Cotovio explains in a companion Genomic Press interview published the same day in Brain Medicine, available at https://doi.org/10.61373/bm026k.0033.
The implications are not academic. If a circuit can produce a symptom, then engaging that circuit, gently and from the outside, might relieve it. Transcranial magnetic stimulation, the non-invasive technique that uses magnetic pulses to nudge cortical activity through the scalp, has been around for decades. What it has lacked is a principled way to choose where to aim. Cotovio's bet is that the lesion-derived circuits are the targets, and that aiming a coil at one patient's individualized connectivity profile rather than at a textbook coordinate is what will turn TMS from a useful but inconsistent treatment into something closer to precision medicine.
The Viewpoint walks the reader through the evidence with the steady hand of someone who has lived inside it. Lesions causing the Capgras delusion, in which a patient becomes convinced that a loved one has been replaced by an impostor, converge on a circuit running through regions implicated in familiarity and belief evaluation. Lesions causing secondary psychosis converge on hippocampal connectivity, and the convergence has already suggested a stimulation target now being trialled. Lesions associated with smoking cessation, which is to say lesions that make people quit, share a connectivity fingerprint involving the cingulate, the insula, and the prefrontal cortex. Veterans with penetrating head injuries who do not develop posttraumatic stress disorder, despite combat exposure that should have produced it, turn out to have damage that intersects a circuit involving the medial prefrontal cortex, the amygdala, and parts of the temporal lobe. The same circuit, remarkably, predicts who will respond to TMS for PTSD in patients with no lesions at all.
The pattern repeats. Mania. Obsessive-compulsive disorder, where Cotovio and colleagues have just extended the framework to lesional cases. Depression, where stimulation sites that relieve the illness and lesion sites that cause it sit on the same functional map. Across diagnosis after diagnosis, the same architectural principle holds. The brain does not store depression in a depression box. It supports adaptive regulation through distributed networks, and when a network buckles, the symptoms that follow depend on which network and which direction.
This reframing, the authors argue, also reshapes what the phrase brain health is supposed to mean. Brain health, in their formulation, is not the absence of disease. It is the capacity of distributed networks to sustain adaptive regulation of emotion, cognition, and behaviour. Resilience to trauma lives in a circuit. So does remission from addiction. So, perhaps, does the everyday business of feeling roughly all right on a Wednesday afternoon. The networks are the level at which genes, lesions, stimulation, experience, and recovery all converge, which is why a framework built on lesions has begun to absorb evidence from deep brain stimulation trials, gene expression atlases, and ordinary functional imaging in patients who never had a stroke at all.
Cotovio came to this work the long way around. Born in Lisbon, where he still lives, he is the son of a psychiatrist, and as he tells it the dinner-table conversations of his childhood circled relentlessly around behaviour and emotion. Medicine pulled him in because it sat at the junction of human stories and biology. Psychiatry held him because it demanded both at once. He earned his medical degree at NOVA Medical School in 2014, joined the Champalimaud Foundation as a research intern in 2015, completed a PhD in Biomedicine in 2023, and finished his psychiatry residency in 2024. Periods at Harvard Medical School with Alvaro Pascual-Leone, Michael D. Fox, and Daniel Press taught him to move between clinic and laboratory, and he has since refused to choose between them. In 2023 he received a Brain and Behavior Research Foundation NARSAD Young Investigator Grant to extend the lesion-network approach to obsessive-compulsive disorder.
He runs in the mornings, when the thinking goes best. He reads. He watches television series with his wife, films with his children. Asked, in the Brain Medicine interview, what he is most proud of, he does not name a paper. He names his family. Asked which living person he most admires, he names his father. His motto, given in Portuguese and translated almost reluctantly into English, is concentração, descontração e vamos para a frente. Focus, calmness, and keep moving forward.
The science is moving forward with him. Whether circuit-informed neuromodulation lives up to its promise will be settled by trials, by replication, by the slow accumulation of evidence that distinguishes a real shift from a fashionable one. Cotovio is the first to insist on the distinction. What he and Oliveira-Maia are arguing, however, is that psychiatry now has, for perhaps the first time in its history, a way to reason about cause in human beings rather than only in animals, and a way to translate that reasoning into where to place a magnet on a particular person's scalp on a particular Tuesday afternoon.
A small stroke, in the right place, can give a person mania. Read backward, that fact is a tragedy. Read forward, it might be a map.
The Brain Health Viewpoint, "From lesions to brain health: Causal circuits in psychiatry," is freely available starting on 5 May 2026 via Open Access at https://url.genomicpress.com/2p8kywb3
The Brain Medicine interview, "Gonçalo Cotovio: Mapping causal brain circuits to personalize neuromodulation in psychiatry," is freely available starting on 5 May 2026 at https://doi.org/10.61373/bm026k.0033. Additional interviews in the Innovators and Ideas series can be found at https://interviews.genomicpress.com/.
About Brain Health: Brain Health is a peer-reviewed journal published by Genomic Press, New York, dedicated to the science and practice of lifelong brain resilience and longevity. The journal publishes original research, reviews, and viewpoints on the biological, clinical, behavioural, and societal dimensions of brain health across the lifespan. Visit https://bh.genomicpress.com/.
About Brain Medicine: Brain Medicine (ISSN: 2997-2639, online; 2997-2647, print) is a peer-reviewed medical research journal published by Genomic Press, New York. The journal publishes work spanning fundamental neuroscience and translational brain medicine, including the underlying science, causes, outcomes, treatments, and societal impact of brain disorders across all clinical disciplines. Visit https://bm.genomicpress.com/.
Genomic Press Virtual Library: https://issues.genomicpress.com/bookcase/gtvov/
Genomic Press media site: https://media.genomicpress.com/
Brain Health: https://bh.genomicpress.com/
Brain Medicine: https://bm.genomicpress.com/
Ma-Li Wong
Genomic Press
mali.wong@genomicpress.com
Visit us on social media:
X
LinkedIn
Bluesky
Instagram
Facebook
Legal Disclaimer:
EIN Presswire provides this news content "as is" without warranty of any kind. We do not accept any responsibility or liability for the accuracy, content, images, videos, licenses, completeness, legality, or reliability of the information contained in this article. If you have any complaints or copyright issues related to this article, kindly contact the author above.